Why Biocelk?
Personalized Diagnosis
Highly Qualified Medical Team and Personnel
Largest and Most Reliable Cell Bank in Latin America
Cutting-edge Technology
Personalized Diagnosis
Highly Qualified Medical Team and Personnel
Largest and Most Reliable Cell Bank in Latin America
Cutting-edge Technology
Explore Treatments
Scientific Literature
Featured Treatments
Wellness & Longevity
Dermo-aesthetic

Fertility
About Biocelk
Our Brands
Visit: regenivf.com
Fertility
Fertility is a complex process that depends on the balance of multiple factors: the quality of eggs or sperm, endometrial health, the hormonal environment, and the body’s ability to sustain a pregnancy.
When any of these elements is affected, difficulties in achieving or maintaining a pregnancy may arise, even after previous attempts with conventional treatments.
At Biocelk®, we approach fertility through regenerative medicine, integrating protocols designed to support specific reproductive functions through biological technologies aimed at improving the cellular environment and promoting more optimal conditions for conception.
Clinical Benefits
At Biocelk®, we open new possibilities in fertility with a regenerative approach designed to help your body respond better and bring you closer to one of the most important dreams of your life.
Endogen Stem Cells
A new possibility when the endometrium seemed unable to respond
When the endometrium is too thin, achieving embryo implantation and moving forward toward pregnancy can become one of the most difficult obstacles in the process. In those cases, it is not only the treatment outcome that worries patients: it is also the feeling of having already exhausted the most common options. Dinorah Hernández and collaborators from Instituto Regenera, Ingenes Mexico, and Cinvestav-IPN published a retrospective dual-arm study in the American Journal of Translational Research (2024) in patients with Asherman syndrome and refractory endometrium, where they evaluated the intrauterine application of autologous mesenchymal cells obtained from the stromal vascular fraction of adipose tissue. After treatment, endometrial thickness improved by an average of 3.2 ± 1.8 mm, and a significant increase was also observed in implantation (66.7% vs 4.8%) and in the live birth rate (47.6%).
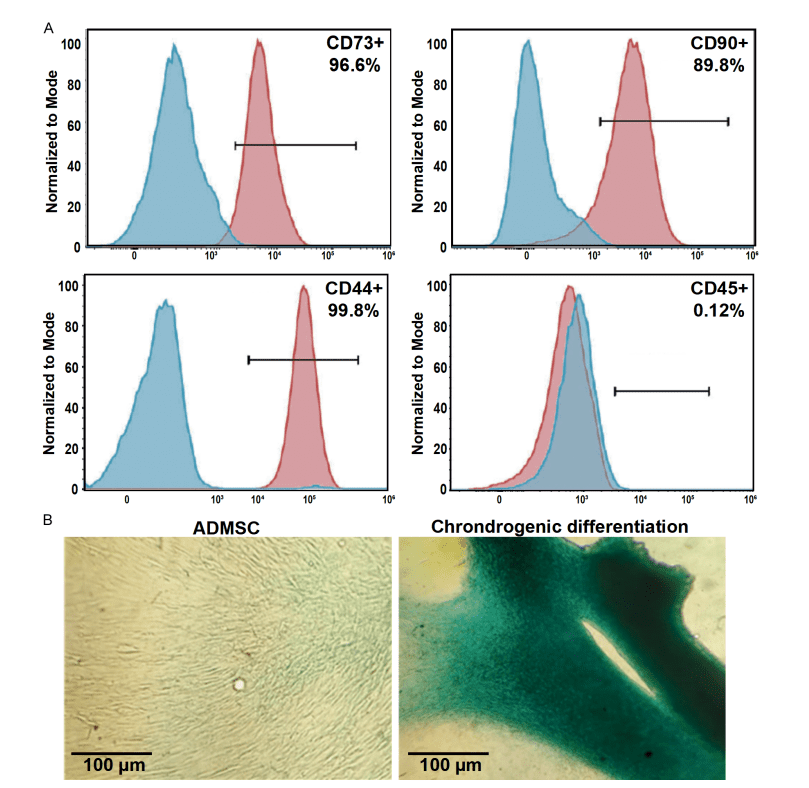
This image documents the biological validation of the cellular component used in the treatment. In the first section, it confirms that the cells display the characteristic profile of mesenchymal cells, recognized for their role in tissue repair and regeneration processes. In the second, it demonstrates their ability to transform into other cell types under specific conditions, supporting their plasticity and therapeutic value. Taken together, the figure does not yet show the clinical result in the patient, but it does show something fundamental: that the treatment begins with a cell population that has real regenerative properties, carefully identified before application.
When you are looking for more options and a different vision of reproductive support, Biocelk® can make the difference.
Endogenous Growth Factors
- 63.9% implantation and 57.4% clinical pregnancy in patients coming from failed cycles
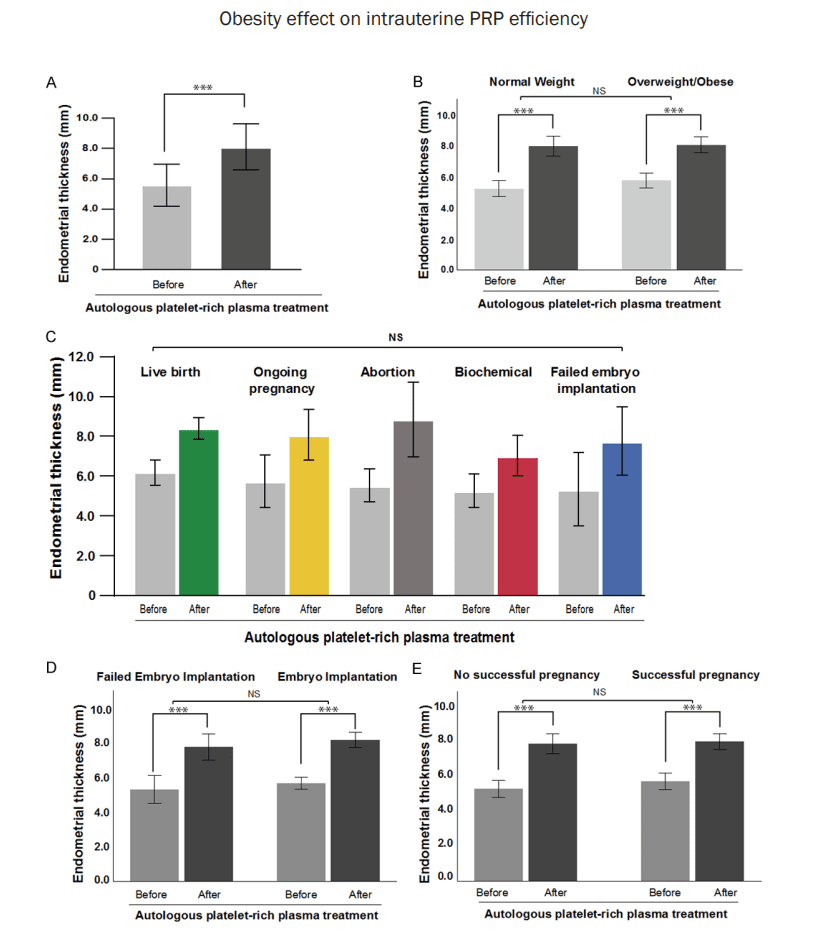
This figure shows that, after intrauterine infusion of autologous PRP, endometrial thickness increased significantly compared to before treatment. Panel A shows the overall change; panel B shows that this improvement occurred both in normal-weight patients and in overweight or obese patients; and panels D and E show that even in women who achieved implantation or successful pregnancy, the endometrium was also thicker after the procedure. In simple terms, this image supports that the treatment helped the uterus become more prepared to receive the embryo.
When the endometrium does not reach the right thickness, each IVF attempt can feel like a mix of hope and exhaustion, especially after several negative results. Dinorah Hernández and collaborators from Instituto Regenera, Instituto Ingenes, and Cinvestav-IPN published a self-controlled retrospective study in the American Journal of Translational Research (2024) in 59 patients with refractory thin endometrium, where they evaluated intrauterine infusion of autologous platelet-rich plasma in a three-dose regimen.
After treatment, endometrial thickness improved by an average of 2.5 ± 1.4 mm, and implantation increased from 22.6% to 63.9%, while clinical pregnancy rose from 16.1% to 57.4%. Although the benefit was lower in overweight or obese patients, the improvement remained significant.
This means the treatment helped the uterus become better prepared to receive the embryo, opening a more realistic possibility where the outlook had previously been limited.
Ovagen
Measurable improvements in reproductive response even after previous failed attempts
The treatment may help create a more suitable environment for embryo implantation, offering a new opportunity in cases where the chances had previously been limited.
At Biocelk®, we can guide you in evaluating whether this approach could become part of your path with scientific support.
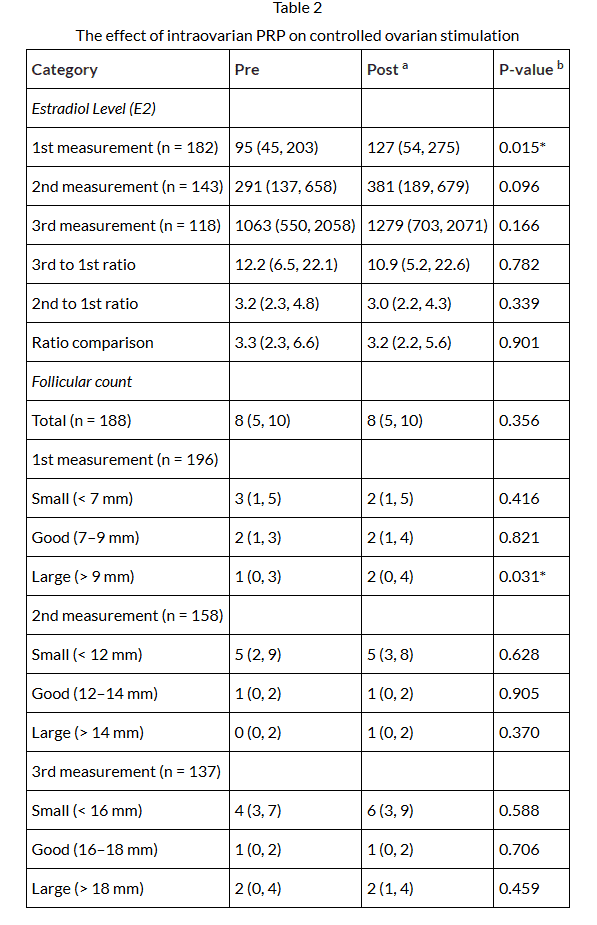
The graphs show a very clear trend: post-treatment values shift toward more favorable ranges compared to baseline. This indicates that the evaluated tissue or system responds positively after application, reflecting a measurable and sustained change throughout the reported follow-up period.
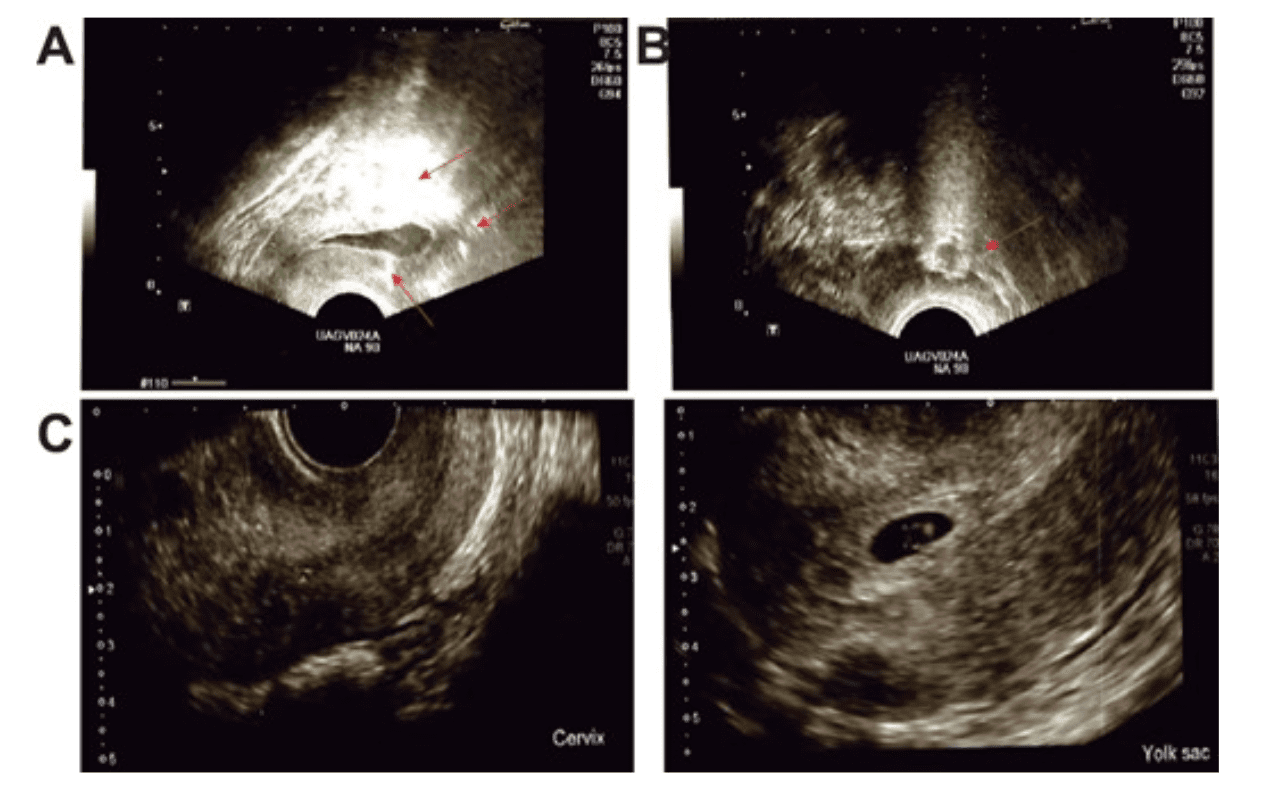
From an endometrium under 5 mm to a full-term pregnancy after regenerative interventions
When you have gone through multiple failed IVF attempts, it is natural to feel that the body is no longer responding and that the options are narrowing. Dinorah Hernández and collaborators published a clinical case in Oxford Medical Case Reports (2023), in which they evaluated a personalized regenerative approach using autologous mesenchymal cells applied to the uterus and later an intraovarian cellular derivative. After two failed cycles with an endometrium under 5 mm, the intervention allowed the endometrium to reach a thickness of 7 mm; later, with the second approach, the development of a euploid embryo was achieved and, after transfer, a pregnancy that reached term with the birth of a healthy baby girl.
Even when the uterine environment and oocyte quality limit success, it is possible to improve key bodily conditions to open new reproductive opportunities.
Testagen
More testosterone and clear improvements in sperm motility
When the diagnosis is severe male infertility, such as oligoasthenoteratozoospermia, it is common to face frustration when sperm parameters do not improve despite conventional treatments.
O Somova and collaborators published a prospective study in Human Reproduction (2021) in men with this condition, where they evaluated the application of an autologous cellular derivative directly into testicular tissue. At 4 months, sperm concentration increased from 1.4 to 4.2 million/ml and motility from 17.7% to 36.7%, with a peak motility increase close to 49.6% at 6 months; in addition, total testosterone rose 2.4-fold compared to baseline.
The treatment may reactivate key biological processes in sperm production and quality, opening new possibilities in cases where the response had previously been limited.
Aumento en la calidad espermática y reducción del daño en el ADN tras el tratamiento.
Biocelk® achieved up to 27.5% sperm recovery in patients who previously had no options
Schedule your evaluation at Biocelk® and discover how a regenerative approach can open new possibilities on your fertility journey.

